Are you curious about your genetic history?
Thanks to modern-day science you have the ability to learn more about your genetic history than ever before.
This article is brought to you in partnership with St. Elizabeth Healthcare.
Curious About Your Genetic History?
I’ve always been curious about my ancestral history… and a little less concerned about my genetic history.
Because of my family’s strong history with cancer, I’ve been apprehensive to face mine.
Part of me dreaded the idea of finding out what I was already aware of. Cancer seems to run in my family, specifically on my mom’s side.
When St. Elizabeth Healthcare invited me to learn more about genetic testing, I was open to learning more.
I faced my fears with my first mammogram, so a meeting to learn more about genetic testing couldn’t hurt right?
Learn More About Genetic Screening Before You Decide to Take the Test
My genetic screening journey began with an appointment with Justine Snyder. She is a Licensed Genetic Counselor at St. Elizabeth Healthcare who helped me understand more about the Genetics program.
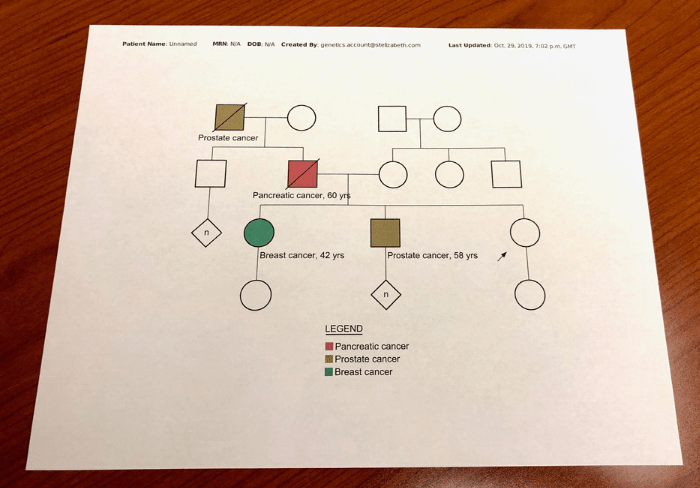
During my appointment, she reviewed my family history, helped to determine if I was a good candidate for genetic testing, what those options are, what the potential results are, etc.
I filled out the genetic screening form to the best of my knowledge. I wished that I would have talked to other family members to get more specifics about cancer in our family. That information really helps build your genetic family tree.
If you have the opportunity, try to ask family members with a history of cancer more about their diagnosis. The type of cancer and the age of their diagnosis can be helpful information to bring to your appointment. If you don’t know or have access to that information, that’s ok too.
During our session, we discussed the multiple generations of affected individuals, their age when they were diagnosed and the types of cancers that can cluster together. The session determined that there are enough features of hereditary cancer risk in my family to warrant the consideration of genetic testing.
I wasn’t surprised by those recommendations because so many family members on my mom’s side have experienced cancer in some form.
You Don’t Have To Decide to do the Genetic Test That Day
After receiving the information, the choice to follow through with the genetic screening was 100% mine.
I decided to take the genetic test for two reasons:
1. I knew that taking a genetic test could save my life. I’m not trying to be overly dramatic here, but I’ve personally seen what cancer can do to someone from watching my mom’s battle with breast cancer.
If my body had a gene that could potentially try to kill me, I want to know about it. Knowing my strong family history with cancer made me want to be proactive in an area that I honestly don’t feel a lot of control over.
My genetic makeup is out of my control, but my response to it with genetic screening is a proactive approach that I can control.
2. I knew taking the genetic test might also help someone reading this article to find the courage to do the screening or at least learn more in an informational session.
That information could also potentially save their life.
The majority of genetic counseling clients do follow through with a genetic test. There are some clients that just want to learn more and others that want to double-check with their insurance before moving forward.
How do they collect your DNA for the Genetic Test?
You have two options for collecting your DNA for the genetic test. They can either draw your blood or they will collect your saliva in a vial.
I do NOT like needles, not that anyone really likes them. I have a fear of needles and avoid them at all costs which made the spit option a no brainer for me.
There is a misconception that your cheek is swabbed for the test. That is NOT what happens with this particular test. (Some tests do allow for a swab.)
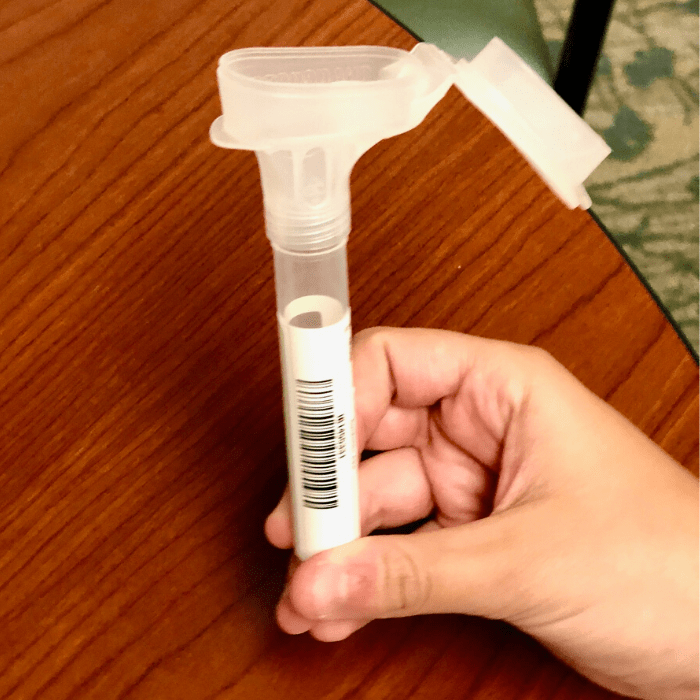
You will need to spit in a vial (pictured above.)
The good news is that the staff step outside of the room so that you don’t have to spit in front of anyone.
*If you are choosing the spit option it’s also important to note that you can’t have anything in your mouth 30 minutes prior to when they gather the DNA sample.
As a frequent gum chewer, that was very important information!
Important Things to Know About Genetic Testing
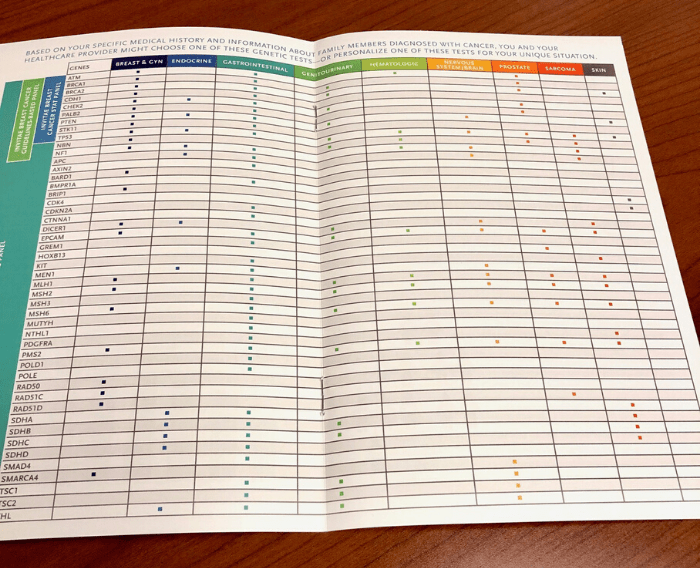
St. Elizabeth provides various genetic screening options depending on your family history and stage of life.
- Hereditary Cancer Testing (For those with a known family history of cancer)
- Preconception and Perinatal Genetic screenings (For those that are pregnant or looking to conceive)
- Proactive Genetic Tests (For those who do not have a strong family history of cancer or cardiac disease).
- Hereditary Cardiovascular Testing
- Pharmacogenomic Testing to see how you metabolize medications
The good news is that new developments and technology improvements have been made in genetic testing. Genetic counselors and specialists can now make risk assessments for hereditary cancer, cardiovascular disease, and many other inherited conditions.
My Genetic Screening Results
The process from start to finish didn’t take very long. The billing department from the lab notified me about my payment options and I received the results within 10 days.
Waiting for the results can seem like an eternity and I tried to keep my mind off of it by focusing on other things.
I did feel comforted by knowing that Justine, my genetic counselor had also been in a similar position and made a proactive choice as a result of her test results. That helped me feel more confident no matter the outcome.
For my specific test, a sample was collected for the Invitae Multi Cancer Panel (84 Genes)
In this case, the test result that I did NOT want was a “POSITIVE.”
A positive means that you have an increased risk of cancer. It was a relief that the BRCA1 and BRCA2 genes common in breast cancer were not found in my results.
I had the option to get my results by phone or in person. My choice was to get the phone call.
Once you have your results, the genetic counselor will help make recommendations for your next steps, if any.
No known clinically actionable alterations (positive mutations) were detected from my test, which was a relief.
My lifetime chance of breast cancer is estimated to be 26.3%, based on the Tyrer-Cuzick (IBIS) risk assessment tool. Women with a risk assessment above 20% meet NCCN criteria for increased breast cancer screening as described below.
A common result and why I still need to be proactive in the future
The test also revealed what is called a genetic variant of uncertain significance (VUS). I was told that in this case, test results are uninformative, or inconclusive.
The vast majority of variants of uncertain significance are later determined to be benign (“harmless.”)
That was a relief to know!
My medical management isn’t impacted by this result. Screening recommendations will be made based on the family history of cancer.
It is vital for me to continue to follow national cancer screening guidelines. I was told that if this variant of uncertain significance is reclassified at a later time, an amended report will be sent to inform me and any additional medical recommendations will be made at that time.
Since the significance of this variant remains uncertain, testing of family members for this variant is not recommended.
However, it was recommended that the family members with cancer, consider hereditary cancer PANEL testing. That test could help with a genetic explanation for cancer occurring in the family that has not yet been identified.
How Do At-Home Genetic Tests Differ From Onsite Genetic Counselors?
Your genetic information needs to be interpreted within your family tree in order to accurately interpret the results.
It can’t stand alone.
So, be careful with some of the at-home genetic tests that provide medical information.
The at-home genetic tests that also provide medical information typically only test for the top few mutations. The problem with that is that there are thousands of mutations that can occur in a single gene, so the vast majority will be missed by at-home genetic tests.
In addition, since the false-positive rate with at-home tests is so high, it is important to confirm all positive at-home results with genetic testing provided by a Genetic Counselor.
Your Genetic Test Results with Support
At. St. Elizabeth Healthcare, the on-site genetic counselors provide support and resources before and after your genetic test. They can help you handle the emotional impact that genetic testing results may have on you or your family.
Genetic screening does not detect the presence of a disease. The test can determine if you are at an increased risk for the disease based on your genetic screening results.
If you’re found to be at higher risk, you may choose to take proactive measures to prevent the disease. Your healthcare team can use your genetic screening results to create a personalized, preventive medical plan of action.
How Much Does Genetic Testing Cost?
The cost of genetic testing can vary depending on your insurance coverage.
I discovered that it was cheaper for me to pay $250 out of pocket. We have a really high deductible and it would have been $1100 with my insurance.
Choose Your Own Genetic Test Adventure
To find a genetic test that is right for you, call 859-301-GENE (4363) or visit stelizabeth.com/dna.
Additional Healthcare Related Articles
What Parents and Students Need to Know About JUULing